Cardiac Molecular Imaging: Overview
In Cardiac Molecular Imaging two techniques are used to assess myocardial viability: SPECT and PET. They both are able to assess myocardial perfusion and / or myocardial function. PET may also be used to evaluate myocardial metabolism.

Cardiac Molecular Imaging: SPECT
Besides analysis of myocardial perfusion and function in gated exams (see chapter function & perfusion), SPECT allows the identification of ischemic but viable myocardium when applying Thallium redistribution studies. The initial uptake of 201Tl depends on regional perfusion, whereas the sustained 201Tl uptake depends on cell membrane integrity and thus myocyte viability. Innovations like IQ SPECT reduce exam time drastically while increasing diagnostic accuracy.

Cardiac Molecular Imaging: PET
Besides analysis of myocardial perfusion and function in gated studies (see chapter function & perfusion), PET allows the identification of viable myocardium. Viable myocardium shows affinity for glucose compared to irreversibly damaged heart muscle. This effect is used in PET imaging. Increased FDG uptake thus indicates viable myocardium. 18F-FDG is the PET tracer to assess myocardial viability. FDG PET is the gold standard for myocardial metabolism assessment (Assessment of Myocardial Viability […]1), its accuracy is increased when using PET/CT.
Cardiovascular MR: Ischemic Cardiomyopathy
Over the last years CMR has been acknowledged as a valuable diagnostic tool for the detection of myocardial viability. LV dysfunction at rest and contractile reserve during the infusion of low-dose dobutamine can be assessed by CMR in a similar way as in echocardiography. In addition, CMR can also be used to assess myocardial perfusion. But most importantly, CMR offers the direct visualization of irreversibly damaged myocardium by a technique called “delayed enhancement” (DE CMR). DE CMR offers better diagnostic accuracy than SPECT, especially for the detection of small and subendocardial infarctions. (Contrast-enhanced MRI and routine SPECT perfusion imaging […]2).
Cardiovascular MR: Subendocardial Septal MI
Therefore DE CMR has become the new gold standard for evaluation of myocardial viability. The major advantage of DE CMR is its superior spatial resolution, which enables differentiation between subendocardial and transmural scars. The basis of DE CMR is the fact that contrast agent accumulates in irreversibly damaged myocardium. This accumulation can be imaged approximately ten minutes after intravenous administration of contrast agent (Myocardial MRI Contrast Agent Concentrations […] 3). DE CMR is of prognostic value before revascularization as can be seen in these two illustrative patients (Cases: Duke University, USA 4). Image quality of DE CMR depends on optimal setting of the inversion time (TI), a parameter which changes during the acquisition. Siemens offers a technique that overcomes this issue: With PSIR delayed enhancement, there is no need for parameter adjustments, which saves time and leads to user independent high image quality. Furthermore, with single-shot PSIR, even patients with arrhythmia can undergo DE CMR imaging. (Assessment of Late Gadolinium Enhancement in Nonischemic Cardiomyopathy […] 5).
Echocardiography
Echocardiography is a valuable tool for evaluation of myocardial viability. Wall thickness and myocardial contractility can easily be evaluated by 2D echocardiography. Low dose Dobutamine stress echocardiography and MCE perfusion studies enhance the determination of myocardial viability. New technologies including instantaneous full volume echo imaging will further improve global assessment of the heart and improve the diagnostic accuracy while reducing examination time.
Cardiac CT
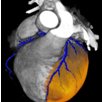
In chronic myocardial infarction the so-called late enhancement phenomen, as described in the Cardiovascular MR chapter, may also be demonstrated in CT. The accuracy of CT late enhancement compares favorable to CMR late enhancement as some initial studies could demonstrate 6). Furthermore CT can be used for assessment of wall thickness and function at rest, which are parameters of myocardial viability. With the Dual Source CT for instance, one scan can give you the coronary status as well as the iodine distribution in the myocardium to answer perfusion questions such as myocardial infarctions and infarct size.
Publications of other clinical experts:
- 1) Schinkel A et al., Journal of Nuclear Medicine 2007, 7: 1135-1146
- 2) Wagner et al., The Lancet 2003; 361:374-379
- 3) Rehwald WG et al., Circualation 2002; 105: 224 - 229
- 4) Cases: Duke University, Durham, USA
- 5) Eklgeti et al., Invest Radiol. 2007 Oct;42(10):671-675
- 6) Brodoefel H et al., Eur J Radiol. 2007;62(2):235-246
Legal Information
A) Data courtesy of University of Michigan, Ann Arbor, MI, USA.
B) Inferoapical infarction. Courtesy of Page-Campbell Cardiology, Nashville, USA.